A while back, I started to become more aware of the language I used to describe Gregory and my journey with Dementia/ Alzheimer's, making sure I always spoke respectfully, articulately, and in a way that did not inappropriately add to the stigma that is often associated with the disease.
In the beginning I didn't even like referring to myself as a "Caregiver" because when you love someone, you do what you have to do to make your lives OK. No label needed! Next, I stared referring to my relationship with Dementia/ Alzheiemr's and Gregory as being part of a "Care Giving Team" which included both Gregory and me. I often referred to the diagnosis as "Our Diagnosis" in that while it was Gregory's illness, I have chosen to walk the path with him.
At Lieberman I am also aware of language use and will carefully, with a large smile, correct people when they use disrespectful or undermining language. For example we use "Cloth Napkins" NOT "Bibs." We use "Paper Pants" not "Diapers." Little things like this make a difference!
Here is Australia's official guidelines for Alzheimer's use language. I saw it on my friend Kate's blog. Writing as a person with Dementia, she has given me a new look, from her angle, of what a person with Dementia experiences. The blog deals becoming more Dementia/ Alzheimer's friendly. Check it out: http://kateswaffer.com/2015/08/24/first-steps-to-being-dementia-friendly/
FOR GREGORY. He was not a VICTIM of ALZHEIMER'S DISEASE, he was a HERO!
PLEASE NOTE: Even though this blog is now dormant there are many useful, insightful posts. Scroll back from the end or forward from the beginning. Also, check out my writer's blog. Periodically I will add posts here if they provide additional information about living well with Dementia / Alzheimer's Disease.
Showing posts with label Language. Show all posts
Showing posts with label Language. Show all posts
Monday, August 24, 2015
The Language of Dementia
Sunday, June 7, 2015
To Use or Not To Use Drugs
Another example Dr. B gave is that Gregory seems to demonstrate a certain level of anxiety, fear, and discomfort if only because he is not able to analyze an experience using language. "That poor guy does not know whether he can trust an experience or if he needs to fear it." You have heard of the very basic "Fight or Flight" instinct.
With the careful, loving use of drugs, I am content in knowing that Gregory does not have to worry about analyzing an experience for fear or trust. Also, he is better able to communicate, using the basic, primitive abilities he has left, to let me (us) know when he is happy, content, sad, or frustrated. And because his responsive behaviors are more under control, we can adjust ourselves to them and make his day to day life as good as possible for him.
Labels:
Aricept,
Drugs,
Exelon Patch,
Fear,
Language,
Namenda,
Responsive Behaviors,
Risperdal,
Trust
Wednesday, May 20, 2015
Wandering or Walking?
Check out Kate Swaffer's poem on "Walking" vs "Wandering." Very expressive!
http://kateswaffer.com/2015/05/21/behaviour-management-or-staff-education/
My reply to her was:
Kate, you did it again.
First, you make it so obvious that words and language can influence how we think, feel, act ... against and for others with Alzheimer's and other dementia related illnesses.
Second, poetry is a wonderful way to express and deal with one's feelings. I have self-published two volumes of poetry many of which are informed by Gregory and my journey through Alzheimer's. When Gregory and I could no longer share language, I turned to my computer to help me process my experiences, frustrations, and emotions which led to beginning my blog and my career as a Poet! I find that often my processing expresses itself through poetry. Other people have said, and I repeat, the poetry writes me not me it!
I have always seen the residents on Gregory's floor and also Gregory as people first and Alzheimer's just as the situation we are in. I have always been careful with my "language" when discussing things about Alzheimer's. But I am getting better at it. I love promoting silly little things like calling a bib a "cloth napkin" and diapers "paper pants."
I have been able to live in their world as well as my own. I have been able to selectively "lie" about "B's" daughter having called to say she loves her. Such joy she felt at such little costs to me!
I have been able to participate in a business meeting to discuss with "J" what we should do about the furniture delivery. Such a sense or purpose for him and what he used to and thinks he still does.
When "S," sitting by the elevator, asks me when her son will arrive, I tell her I am not sure but I see if I can find out.
But you have brightened my outlook on seeing the entire disease in a new way and how to treat and care for my fellow human beings according to how we talk about dementia and the people affected by it (both those with dementia and those who love and care for them.)
I have begun informing, educating, correcting, etc people with whom I come into contact when their language seems inappropriate. I do so gently and with love. Tonight at dinner, the sister of "M" shared with me that "M" has been aggressive today. I asked, "Is it aggressive or energetic?" The sister liked that and repeated, "Yes, energetic."
If I may, this is my BLOG: http://mhorvichcares.blogspot.com
Also, if I may, this is where my poetry is available: http://www.amazon.com/s/ref=nb_sb_noss?url=search-alias%3Daps&field-keywords=michael+horvich
(P.S. If you buy a new new one, the profits go to Gregory's Lieberman Center Alzheimer's Special Care unit. The used ones available at a cheaper price are owned by others and their profits are not shared.)
Labels:
Attitude,
Language,
Lying,
People First,
Poetry
Monday, May 18, 2015
Whose Story Is It?
I continue to follow and learn from Kate Swaffer, a professional diagnosed with dementia who lives in Australia. Check out her latest blog, "Who's Story is It?" http://kateswaffer.com/2015/05/19/whos-story-is-it/
These are my comments to her:
For one, I am very excited about two seemingly current movements: 1) Being more careful with "language" when describing people with dementia and recognizing that many of the "Inappropriate Behaviors," "Violence," "Acting Out," etc are more indicators of discomfort, fear, frustration, etc of not being able to communicate using the vary language that we so carelessly use! 2) Hearing from more people who have been diagnosed with dementia is so important to get a REAL picture of what is going on in their lives and on how they are and/or should be treated and cared for. I have to admit that as an educated, knowledgeable, caring person I almost didn't see being a care giver from that angle. In my case, Gregory was unable to communicate his needs but I did know him so well after 40+ years of a wonderful relationship I was able to know (for the most part) and meet his needs in a loving, respectful, honorable way. Thanks Kate for being there!
These are my comments to her:
For one, I am very excited about two seemingly current movements: 1) Being more careful with "language" when describing people with dementia and recognizing that many of the "Inappropriate Behaviors," "Violence," "Acting Out," etc are more indicators of discomfort, fear, frustration, etc of not being able to communicate using the vary language that we so carelessly use! 2) Hearing from more people who have been diagnosed with dementia is so important to get a REAL picture of what is going on in their lives and on how they are and/or should be treated and cared for. I have to admit that as an educated, knowledgeable, caring person I almost didn't see being a care giver from that angle. In my case, Gregory was unable to communicate his needs but I did know him so well after 40+ years of a wonderful relationship I was able to know (for the most part) and meet his needs in a loving, respectful, honorable way. Thanks Kate for being there!
Labels:
Dementia Identified,
Kate Swaffer,
Language,
Stories
Tuesday, May 12, 2015
Interesting how this is beginning to show up. In summery, "How we talk about Alzheimer’s and other dementias has a profound effect on how we perceive and deal with the illness.”
Interesting how this is beginning to show up more and more or am I just tuning in? I know you have been talking about this for a while.
I too believe how we talk about Alzheimer’s and other dementias has a profound effect on how we perceive and deal with the illness.
I just reviewed all of the descriptors on my blog (which just passed 50,000 hits with 178 posts) http://mhorvichcares.blogspot.com
I was pleased (and somewhat amazed) to find that most of the negative descriptors were more about how I was dealing or "suffering" through being a caregiver for my life partner of 40+ years Gregory.
I did compare some days to "being in hell," suffering, experiencing Gregory's violence towards me and a few others, feeling out of control, dealing with this "insidious" disease, feeling flummoxed.
My use of words and attitudes towards Gregory and his dealing with the disease were mostly positive and reflect something I have been saying from the beginning, "Gregory is NOT a VICTIM of Alzheimer's, he is a HERO!"
Michael
Monday, August 18, 2014
This Evening at Lieberman
I spent three hours with Gregory today.
From 2:00-3:00, Barbara, a volunteer, played piano. I think she is older than many of the residents on the floor and her energy, or lack of it, showed in her playing.
I am not criticizing, just describing. Many residents slept, many stared, a few clapped their hands or sung. Each, in their own way, enjoyed the performance.
Back in Gregory's room, we partook of some of the food treats I had brought in: pitted cherries, fresh figs, animal cookies, refrigerated chocolate covered mini donuts, and pretzel rods.
The way to Gregory's heart is through his mouth ... really! Manny was placing a cherry on Gregory's specially handled and weighted fork and Gregory was methodically able to bring the cherry to his mouth, pull it off with his teeth, and enjoy the wonderful taste with his eyes closed.
At one point I asked Gregory to give me a cherry. It was already skewered onto his fork, I put my face close enough to him and he actually put a cherry in my mouth! Oh joy!
Later when I gave him a pretzel rod, I labeled it out-loud to him, "Pretzel! Can you say that." Without much thinking, Gregory responded, "Pretzel." Manny and I were elated, applauded, and Gregory smiled.
Gregory noticed the photograph of Julia Child which sits in a black frame on his window sill. "Oh wow!" he said, as if discovering not only the photo for the first time but also the memory's return for the first in a long time. Tears (of joy) came to him and I gave him a hug. I asked if he wanted me to tell the story? He shook his head, "Yes."
I proceeded to retell the story of how Julia Child used to live in the same neighborhood as Gregory when he lived in Boston. They used to run into each other at the butcher and developed an acquaintanceship over discussing the various cuts of meats. Gregory has always prided himself in this story and told it many times over when he was able.
On listening to my retelling with rapt attention, the tears flowed in abundance with the look of such pain, longing, remembering, being overwhelmed, uncontrollable grief, not sure exactly which emotions were really present.
I hugged him and we rocked and cried together. Sometimes I am grateful that Gregory still has emotions and is able to express them but this time I wondered if the pain was worth their recalling.
A little later he started calling, "Momma ... momma ... momma." He did this chain of three several times and the tears began again. I am not sure what prompted this or why and according to Manny, it was a first. We rocked and cried again.
Now that it was getting close to dinner time I decided I needed to try to cheer him up so I asked him if he wanted me to do "The Teddy Bear Puppet Show?" He responded by shaking his head, "Yes."
His Teddy Bear, named Peaceful, is large enough and flexible enough that when grabbed by the back of its neck, one can do a pretty good imitation of having the bear dance, sing, act silly, wave, give kisses, whatever.
So we did the usual show, Gregory began to smile, kissed Peaceful in return, and we all broke into giggles as how silly I was being.
The other day, during a similar puppet show, Gregory instead of kissing the bear, grabbed its nose in his mouth, bit hard, shook his head back and forth, and "Gurrrrrrred" as if he was a bear himself.
The Teddy Bear's name is "Peaceful." "Peaceful," Gregory repeated and we went off to dinner.
From 2:00-3:00, Barbara, a volunteer, played piano. I think she is older than many of the residents on the floor and her energy, or lack of it, showed in her playing.
I am not criticizing, just describing. Many residents slept, many stared, a few clapped their hands or sung. Each, in their own way, enjoyed the performance.
Back in Gregory's room, we partook of some of the food treats I had brought in: pitted cherries, fresh figs, animal cookies, refrigerated chocolate covered mini donuts, and pretzel rods.
The way to Gregory's heart is through his mouth ... really! Manny was placing a cherry on Gregory's specially handled and weighted fork and Gregory was methodically able to bring the cherry to his mouth, pull it off with his teeth, and enjoy the wonderful taste with his eyes closed.
At one point I asked Gregory to give me a cherry. It was already skewered onto his fork, I put my face close enough to him and he actually put a cherry in my mouth! Oh joy!
Later when I gave him a pretzel rod, I labeled it out-loud to him, "Pretzel! Can you say that." Without much thinking, Gregory responded, "Pretzel." Manny and I were elated, applauded, and Gregory smiled.
Gregory noticed the photograph of Julia Child which sits in a black frame on his window sill. "Oh wow!" he said, as if discovering not only the photo for the first time but also the memory's return for the first in a long time. Tears (of joy) came to him and I gave him a hug. I asked if he wanted me to tell the story? He shook his head, "Yes."
I proceeded to retell the story of how Julia Child used to live in the same neighborhood as Gregory when he lived in Boston. They used to run into each other at the butcher and developed an acquaintanceship over discussing the various cuts of meats. Gregory has always prided himself in this story and told it many times over when he was able.
On listening to my retelling with rapt attention, the tears flowed in abundance with the look of such pain, longing, remembering, being overwhelmed, uncontrollable grief, not sure exactly which emotions were really present.
I hugged him and we rocked and cried together. Sometimes I am grateful that Gregory still has emotions and is able to express them but this time I wondered if the pain was worth their recalling.
A little later he started calling, "Momma ... momma ... momma." He did this chain of three several times and the tears began again. I am not sure what prompted this or why and according to Manny, it was a first. We rocked and cried again.
Now that it was getting close to dinner time I decided I needed to try to cheer him up so I asked him if he wanted me to do "The Teddy Bear Puppet Show?" He responded by shaking his head, "Yes."
His Teddy Bear, named Peaceful, is large enough and flexible enough that when grabbed by the back of its neck, one can do a pretty good imitation of having the bear dance, sing, act silly, wave, give kisses, whatever.
So we did the usual show, Gregory began to smile, kissed Peaceful in return, and we all broke into giggles as how silly I was being.
The other day, during a similar puppet show, Gregory instead of kissing the bear, grabbed its nose in his mouth, bit hard, shook his head back and forth, and "Gurrrrrrred" as if he was a bear himself.
The Teddy Bear's name is "Peaceful." "Peaceful," Gregory repeated and we went off to dinner.
Labels:
Emotions,
Food,
Language,
Lieberman,
Memories,
Music,
Sense of Humor,
Silly,
Sorrow,
Tears,
Teddy Bear
Friday, November 22, 2013
A New Language
As you know, Gregory has difficulties with language retrieval as well as generation not to mention connections between words and their meanings and/or associations. When he is focused on an item, no words or pointing can distract him from that focus. So if you say "Give me the fork," often he can. But if he is looking at or thinking about a glass, you can "fork" until you are blue in the face and you'll only get "glassed!" Got it?
Meanwhile, I realized recently that we have been creating a new language that we use more successfully. When he gets undressed at night, I stand at the closet to collect his clothes to be hung up for the next day. Often he puts the item of clothing being taken off on the bed ... or on the bench ... or on the floor. When I say "Hammy" (a verbally joined together combination of "Hand it to me," he seems to understand and hands me the item of clothing.
He will take off most of his clothing but then get distracted or not realize that he still has on his underpants, undershirt, and/or sox. So I say, "Take off more" followed by "Hamme" and he takes off the next item of clothing and gives it to me. I continue this until he is standing there nude. Then I hand him his night clothes and he usually knows what to do with them.
Often he takes the night clothes into the bathroom because it is warmer in there, puts on the top or bottom, depending, and comes out of the bathroom not realizing or knowing that he still has the bottom or top, depending, to put on. I point and say "You stopped!" and he gets it.
Why does this new language work? I do not know, but I will be more aware of it and see how many new words I can add to make our life a little easier.
Meanwhile, I realized recently that we have been creating a new language that we use more successfully. When he gets undressed at night, I stand at the closet to collect his clothes to be hung up for the next day. Often he puts the item of clothing being taken off on the bed ... or on the bench ... or on the floor. When I say "Hammy" (a verbally joined together combination of "Hand it to me," he seems to understand and hands me the item of clothing.
He will take off most of his clothing but then get distracted or not realize that he still has on his underpants, undershirt, and/or sox. So I say, "Take off more" followed by "Hamme" and he takes off the next item of clothing and gives it to me. I continue this until he is standing there nude. Then I hand him his night clothes and he usually knows what to do with them.
Often he takes the night clothes into the bathroom because it is warmer in there, puts on the top or bottom, depending, and comes out of the bathroom not realizing or knowing that he still has the bottom or top, depending, to put on. I point and say "You stopped!" and he gets it.
Why does this new language work? I do not know, but I will be more aware of it and see how many new words I can add to make our life a little easier.
Saturday, April 13, 2013
Gregory's Meditation Session One
Yoga Nidra with Corinne Peterson has been so beneficial for me that I decided to see if it would be of benefit to Gregory. The concept was not to follow Yoga Nidra exactly, but to allow Gregory some "time away from himself." Often he is frustrated when he can't tell you what he is thinking, or he struggles to figure out how to cut a piece of meat or brush his teeth. The more time we can allow him free from pain, distraction, frustration etc the better. So we are calling this, as we have called other experiences, "A Nobel Experiment."
Corinne and I began an e-mail dialogue on what a Practice (yoga session) might look like for someone with Alzheimer's. We needed to take into consideration language and communication difficulties, Gregory's inability to focus on complicated directions, and other Alzheimer's issues. We were concerned that he would not be able to give us feedback on the process.
Following are some of the thoughts Corinne and I shared:
Corinne,
Corinne and I began an e-mail dialogue on what a Practice (yoga session) might look like for someone with Alzheimer's. We needed to take into consideration language and communication difficulties, Gregory's inability to focus on complicated directions, and other Alzheimer's issues. We were concerned that he would not be able to give us feedback on the process.
Following are some of the thoughts Corinne and I shared:
"We've talked a little about what the session on Thursday might feel like. Here are a few more thoughts and suggestions. I am just thinking out loud, you are the expert in Yoga Nidra, I am somewhat the expert in Alzheimer's although Gregory is the real expert in Alzhiemer's, just unable to share his expertise.
Use less detail. Start at head and work your way down to toes but do so simply. For example "be aware of your mouth." Don't complicate it by "left mouth" "right mouth" "top of mouth" "bottom of mouth." etc. Lips-OK, Tongue-Ok, Teeth-Ok for example but leave the detail out?
Hands - OK. Fingers - OK but leave out left and right. Leave out thumb, pinkie, ring finger, etc. Allow enough space for him to process the suggestions made. We will have to play this one by ear, maybe his face will cue us?
Hands - OK. Fingers - OK but leave out left and right. Leave out thumb, pinkie, ring finger, etc. Allow enough space for him to process the suggestions made. We will have to play this one by ear, maybe his face will cue us?
For 5 breathing and noticing in and out is good. A countdown from 12 to 1. Gregory cannot count by himself. Instructive: "We will count our breaths down from 12. Breath in, breath out 12. Breath in, breath out 11. etc. Our breathing could be loud enough to guide him as you cue.
For 6: one or two emotions. Happiness and Sadness for example. After suggesting the emotion, maybe let Gregory create his own thoughts during the silence instead of complicating it by offering options or alternatives. Then go to Sadness and let him create what makes him sad. Then come back to happiness and leave it on the positive note. Maybe the word itself will be enough for Gregory to think about.
End with a guided imagery through a forest. Suggest the images leaving a lot of quiet space for him to process. Something like "Lets be quiet for a while and think about a forest." His processing is so slow that the space is important. Perhaps offering generalities of a forest and again allow space for his processing would help. Picture the trees...... Do you see the sun shining through the trees... Picture the path..... Do you see any animals.....
Allowing the right amount of space for him to process the suggestions is important. Not too much. Not too little. We will have to play this one by ear, maybe his face will cue?
Corinne, based on our conversations the last few times, how does all this sound to you? The goal is to tailor the session to Gregory. I am just coming along for the ride so don't worry about making it meaningful for me. I will probably have as my intention to entrain with Gregory to "feel" how it is going for him.
Looking forward to the session.
• • • • •
Corinne,
Thanks for today. I think it was a great success. Your pacing was perfect as was your simplicity of suggestion. We do not need to know exactly what Gregory experienced in detail but I think his "waking" reactions were very telling as to your success. (Two thumbs up. "Wonderful." "Amazing." I was SO PLEASED! Did you notice the tears in my eyes? Joy!
Michael
Corinne shared an e-mail that Richard Miller sent in answer to someone's query about Yoga Nidra and people with dementia. He is the guru of Yoga Nidra and her teacher. It was interesting to see how what he had to say overlapped Corinne and my discussions.
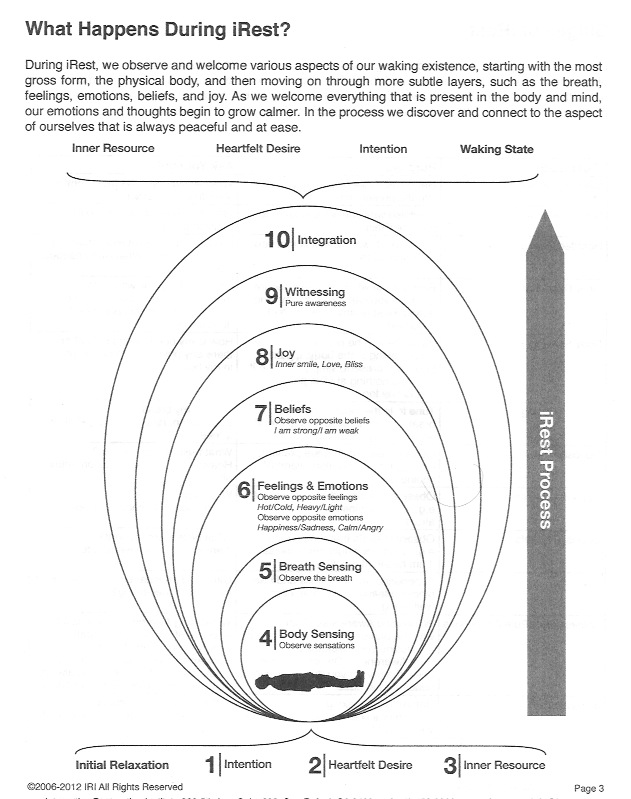
iRest (Yoga Nidra) for this particular group is a wonderful offering, especially when delivering certain aspects of the practice that are sensate oriented, such as body sensing and breath awareness.
These practices are focused in the here and now, and can help this population feel at ease and calm. Also imagery can be a useful aspect by bringing in images that the individuals give you and speaking them back, like you are taking them on a beautiful and present focused journey.
I also think any way to interweave joy through things like chocolate meditations, smelling flowers, holding hands in the heart to evoke feelings of love, etc., can be wonderful elements to weave into a practice.
Using hands on materials like we do with kids, i.e., cloth or textures to touch, things to smell (floors) or hear (bells) or see (die settling into a water vase.)
The sky is the limit. Just our imagination as teachers as to what we can bring to enliven the senses, nourish the felt sense of being and being in the hare an now, etc.
Michael
Corinne shared an e-mail that Richard Miller sent in answer to someone's query about Yoga Nidra and people with dementia. He is the guru of Yoga Nidra and her teacher. It was interesting to see how what he had to say overlapped Corinne and my discussions.
iRest (Yoga Nidra) for this particular group is a wonderful offering, especially when delivering certain aspects of the practice that are sensate oriented, such as body sensing and breath awareness.
These practices are focused in the here and now, and can help this population feel at ease and calm. Also imagery can be a useful aspect by bringing in images that the individuals give you and speaking them back, like you are taking them on a beautiful and present focused journey.
I also think any way to interweave joy through things like chocolate meditations, smelling flowers, holding hands in the heart to evoke feelings of love, etc., can be wonderful elements to weave into a practice.
Using hands on materials like we do with kids, i.e., cloth or textures to touch, things to smell (floors) or hear (bells) or see (die settling into a water vase.)
The sky is the limit. Just our imagination as teachers as to what we can bring to enliven the senses, nourish the felt sense of being and being in the hare an now, etc.
Labels:
Communication,
Language,
Meditation,
Reactions,
Simplicity,
Success,
Yoga
Tuesday, April 2, 2013
Companion Report #2 by K.C.
It’s been approximately 12 months since I first met Greg and his symptoms seem to be gradually getting worse. Below are some changes I’ve noticed in Greg, as well as things that still seem to remain the same. I should note, however, that my observations are highly subjective.
Things that seem to have changed:
Greg’s capability of using words has declined slightly. Words do not come out as he wishes, and he frequently makes mistakes even when they do come out. Sometimes, the word itself is correct, but it is not the right choice. For example, when I went painting with him, he said “red” looking at “blue”, and this happened a number of times. Other times, he struggles saying words. For instance, he said “pint, pinkle…” when he meant to say “pink”. His struggle for words is not anything new, but it seems to me that the frequency has slightly increased.
He needs more assistance in everyday life activities (getting dressed, preparing lunch, cleaning up, etc.). He gets confused, disoriented, and even simple tasks can tire him out.
It seems like his hands shake more often than before. This is especially noticeable when he is trying to bring food or drink to his mouth.
His dependence on me has increased. This has to do with him needing more help, but also his feeling more comfortable around me. For example, he might tell me “you do it!” when I’m trying to explain how to put on his scarf before we go out.
He might get tired more easily than before. After we go for a walk, it seems like we always speak about how tired we are.
Some routines he had little trouble with several months ago are getting more difficult for him. I was surprised when he asked me to make his lunch for the first time. He used to put together a nice salad for himself, but now it seems as though he lacks the confidence to do so. However, I would suggest that his forgetfulness has not happened over night, and it seems to do with how long it has been since he last made lunch. Apparently, it had been quite some time since he last made his salad, which may play a role in why he forgot how to do it.
Things that seem to remain the same:
I have never noticed any changes in his personality. He also does not have mood swings either, and he is still the same Greg that I know.
I have never noticed Greg hallucinating. His sense of smell, sight, hearing, still remains the same. Perhaps delusion is not the right word, but there are certain things Greg believes, which are unrealistic. For example, he believes that Meryl Streep lives near by (I haven’t checked whether this is true or not, but seems unlikely). I’ve heard this a number of times from Greg.
Memories from the distant past seem to remain pretty much the same.
He can still sympathize and understand what others are feeling. For example, when I was talking to Michael about how a package sent from Japan was stolen, Greg knew how upset I was and he sympathized appropriately.
Although Greg sometimes forgets to flush the toilet, I’ve never helped him use the bathroom. He goes to the bathroom when he wants, and he has never asked for help.
Although he doesn't remember people’s names, he still recognizes them. Occasionally, we bump into somebody we know—or somebody he knows, but he always recognizes them, which is a good sign.
We can still communicate even though he cannot express what he wants to say perfectly.
His walking speed has not changed, and he has no problem swimming.
I have not noticed any decline in his appetite, and he still eats quite a lot.
Although I do not know how much he understands what he reads in the newspaper, he still sits down and reads it.
Labels:
Appetite,
Changes,
Comprehension,
Daily Routine,
Dependence,
Empathy,
Face Recognition,
Hallucinations,
Language,
Life Skills,
Memories,
Personality,
tired
Subscribe to:
Comments (Atom)